Stress Fracture Support Services
Stress fractures can occur in various parts of the body. Common stress fracture locations include:
- Distal second metatarsal
- Navicular
- The shaft of the tibia
- The base of the fifth metatarsal
Stress fractures differ from standard fractures as they are not complete breaks in the bone. Instead, they are small stress lines or cracks caused by repetitive strain. They are commonly triggered by physical activities.
At Orthotics Plus, we treat most types of stress fractures at our Melbourne clinics.
Symptoms of Stress Fractures
Symptoms/onset of stress fractures typically manifests as follows:
- A result of repetitive, strenuous activities like running and jumping.
- Initially, the main symptom is localised pain, which is commonly described as a “hotspot.” The pain is sometimes referred to as a “hotspot” because it can be identified through imaging, such as blood flow imaging that highlights areas of inflammation.
- The pain is typically the first sign and may worsen during activities but improve during rest.
- If the condition is not managed properly, the stress fracture can progress.
- People often attempt to push through the pain or continue running despite discomfort.
- Other accompanying symptoms include swelling and tenderness in a specific spot.
- The tenderness can be quite specific, and touching the affected area will elicit pain.

Treatment of Stress Fractures
The overall strategy for stress fractures, and indeed most types of fractures involves:
- Immobilisation methods such as moon boots, rigid sole shoes, and carbon fibre stiffening
- In the case of tibial stress fractures, CAM boots or moon boots are recommended.
- Arch support is often provided for navicular fractures, especially in patients with pronation or collapsed arches, as this helps reduce stress on the navicular bone.
- Immobilisation techniques are used to minimise movement and promote healing.
- Activity modification plays a crucial role in treatment by reducing the load and impact on the injured site.
- Gradual return to activity during the recovery phase, starting with walking and progressing to activities like running in intervals (e.g., a minute on, minute off). This approach helps prevent the recurrence of stress fractures.
At Orthotics Plus, we provide professional fracture management services and work with your healthcare team to develop an appropriate rehabilitation plan. The typical timeline of treatment is between 6-12 weeks, though this can vary.

Mitigating the Recurrence of Stress Fractures
To prevent and mitigate stress fractures, Orthotics Plus recommends:
- Foot postural factors play a role in stress fractures, particularly in navicular and distal second metatarsal fractures. For individuals with pronated feet or forefoot overload due to conditions like bunions or stiffness in the great toe, offloading will be necessary. Orthotics can be used to provide support and prevent injury recurrence.
- Over-pronation can create torsion through the tibia, so orthotics may be beneficial in some cases, although not necessary for everyone.
- Footwear selection is a large factor. It should provide appropriate support based on foot posture and activity levels. The ideal shoe varies from patient to patient.
- As mentioned, gradual progression is essential, avoiding sudden excessive load on the bones, such as attempting to run a full marathon without appropriate training. Allowing the bones to adapt to the load over time is recommended.
In summary, mitigating stress fractures involves the management of biomechanics, load management and footwear.

Who Is Affected By Stress Fractures?
The common denominator for patients with stress fractures is activity or an increase in activity.
This includes active people returning to physical activity after a period of time. For instance, those who have taken time off due to pregnancy and are resuming activities like running or playing sports as an adult, especially those who start running later in life.
This was evident during the Covid-19 lockdowns, when people were home and gyms were closed. Many took up running and extended walking on footpaths and hard roads and we witnessed an increase in stress fractures.
Conditions like bunions, osteoporosis or hallux rigidus (stiffness in the great toe) can lead to overload on the second metatarsal, causing stress fractures. Furthermore, individuals with a pronated foot posture may have a higher likelihood of experiencing tibial stress fractures or navicular stress fractures.
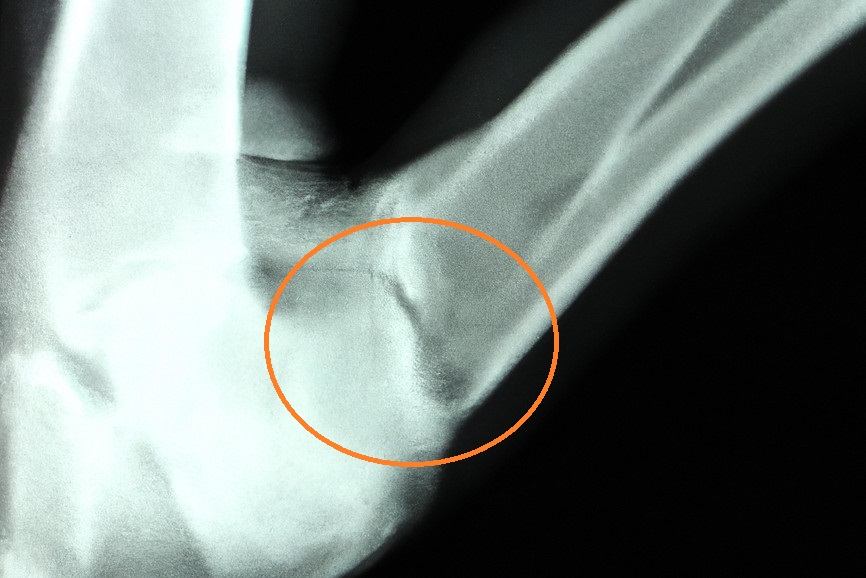
Diagnoses
Stress fractures are diagnosed through a combination of clinical evaluation, patient presentation and imaging scans.
Due to their small size, it can be challenging to detect stress fractures based solely on an assessment. However, certain factors can raise suspicion of stress fractures.
When a patient presents with pain, an anecdotal description of their injury and swelling in a prevalent location of a fracture, we as Orthotists would likely be suspicious of a stress injury.
We will also enquire about your activity levels and if you have started doing more.
To confirm the diagnosis, imaging scans are typically used. X-rays may not always reveal stress fractures in the early stages, but they can help rule out other conditions. MRIs are more sensitive and can detect subtle changes in the bone that indicate a stress fracture.
Rarely, a Positron Emission Tomography (PET) scan can be considered to evaluate bone metabolism and activity, providing information about increased metabolic activity that could indicate stress fractures or areas of healing.
Contact Us for Stress Fracture Support Today
Take action if you’re experiencing unexplained pain that intermittently arises during activities. It’s crucial to investigate the underlying cause and seek appropriate management early.
With our extensive experience in dealing with stress fracture patients, we have established strong connections with physiotherapists, sports doctors, and orthopedic surgeons to ensure comprehensive fracture management services.
Contact any of our clinic locations in Melbourne to book an appointment and receive appropriate treatment for your injury.
