Contracture Management Services
At Orthotics Plus, we provide professional contracture management services.
Various neurological conditions can contribute to contractures, such as strokes, cerebral palsy, ABI.
Additionally, orthopedic traumas, like fractures, can also lead to contractures. For example, an elbow fracture that requires immobilisation can cause a contracture in the biceps, limiting the ability to achieve full extension.
At Orthotics Plus, we offer conservative management services to address and alleviate contractures, helping patients regain better mobility and joint function

What Are Contractures?
Contractures can be classified into two main categories:
Physical contractures:
- These contractures typically result from injuries where a limb or joint remains stuck in a particular position.
- The capsule surrounding the joint becomes stiff, and the muscles atrophy, leading to limited mobility and joint binding.
- Management for physical contractures involves a combination of physiotherapy and possibly bracing or splinting to gradually improve the stiffness over time.
Neurological contractures:
- Neurological contractures are often associated with conditions like stroke, cerebral palsy, or other brain-related issues.
- The brain continuously sends signals to a muscle, causing it to contract persistently, resulting in the muscle getting stuck in that position.
- This high tone in the affected muscle and stiffness in other muscles can lead to joint stiffness as well.
- Managing neurological contractures requires a different approach. Simply using braces might not address the root cause, and the contracture can recur.
- Treatment for neurological contractures may involve Botox injections, tendon lengthening, or other interventions to target the underlying cause combined with orthotic management.


How Contractures Impact Daily Life
Contractures are often ever present, causing a joint to remain locked in a fixed position unless physically manipulated. They can affect people at all hours of the day, typically symptoms and consequences include:
- Pain and discomfort
- Loss of mobility and range of motion
- Affected daily tasks and self-care
- Difficulty performing functional activities
- Risk of secondary complications (e. muscle imbalance, increased severity)
- Effect on mental health
- Occupational and social considerations
Contractures do not occur intermittently and are different to spasticity; they are either present or absent. For instance, if a joint is stuck in a bent position and cannot be straightened, it is considered a contracture, restricting the joint’s range of motion and functional abilities.
The severity and location of the contracture determine its impact on daily life. A minor contracture, such as a slight deviation in knee alignment due to a previous ACL injury, may have minimal effects on daily activities.
However, a significant contracture, where the knee is constantly stuck at 120 degrees of flexion, can severely impair day-to-day function.
Spasticity can be linked to contractures:
Individuals with spastic muscles may face challenges in straightening the affected limb, leading to reflexive contractions.
Spasticity can contribute to the development of contractures, characterised by a restricted range of motion at a joint due to muscle tightness.
Long term outcomes
The curability of contractures depends on the underlying cause, severity, and the individual’s response to treatment. In some cases, contractures can be fully or partially reversed, while in others, they may be managed but not completely cured.



Diagnoses and Treatment
In the diagnosis and treatment of contracture management, Orthotists often collaborate with physiotherapists to address cases where patients may not be improving with standard physiotherapy alone.
Diagnosis:
Contractures are typically diagnosed by physiotherapists who work closely with the patients and observe their progress over time.
Patients who show limited improvement or need extra assistance may be referred to Orthotists for intervention.
Treatment Approach:
- The primary approach in contracture management is slow and prolonged stretch to encourage joint mobility.
- For example, in elbow flexion contractures, our Orthotists may recommend using a splint with an active extension force overnight for an extended period (e.g., 10 hours). This helps gradually encourage the extension of the elbow joint.
- Similarly, knee flexion contractures, often observed in wheelchair-bound individuals, are managed by promoting knee extension for an extended period.
- Calf contractures, where individuals have difficulty placing their heels on the ground when standing, are addressed using Ankle-Foot Orthotics (AFOs) or similar devices that encourage dorsiflexion.
Collaboration with Physiotherapists:
- Orthotists work in close coordination with Physiotherapists, leveraging their expertise to complement and enhance the overall treatment plan.
- This collaborative approach ensures that the treatment aligns with the patient’s specific needs and conditions.
- By combining Orthotic interventions with Physiotherapy, patients can receive comprehensive care that maximises their chances of improving joint function and mobility.
The professional application of Orthotic devices, combined with physiotherapy, can lead to positive outcomes and improved quality of life for individuals with contractures.
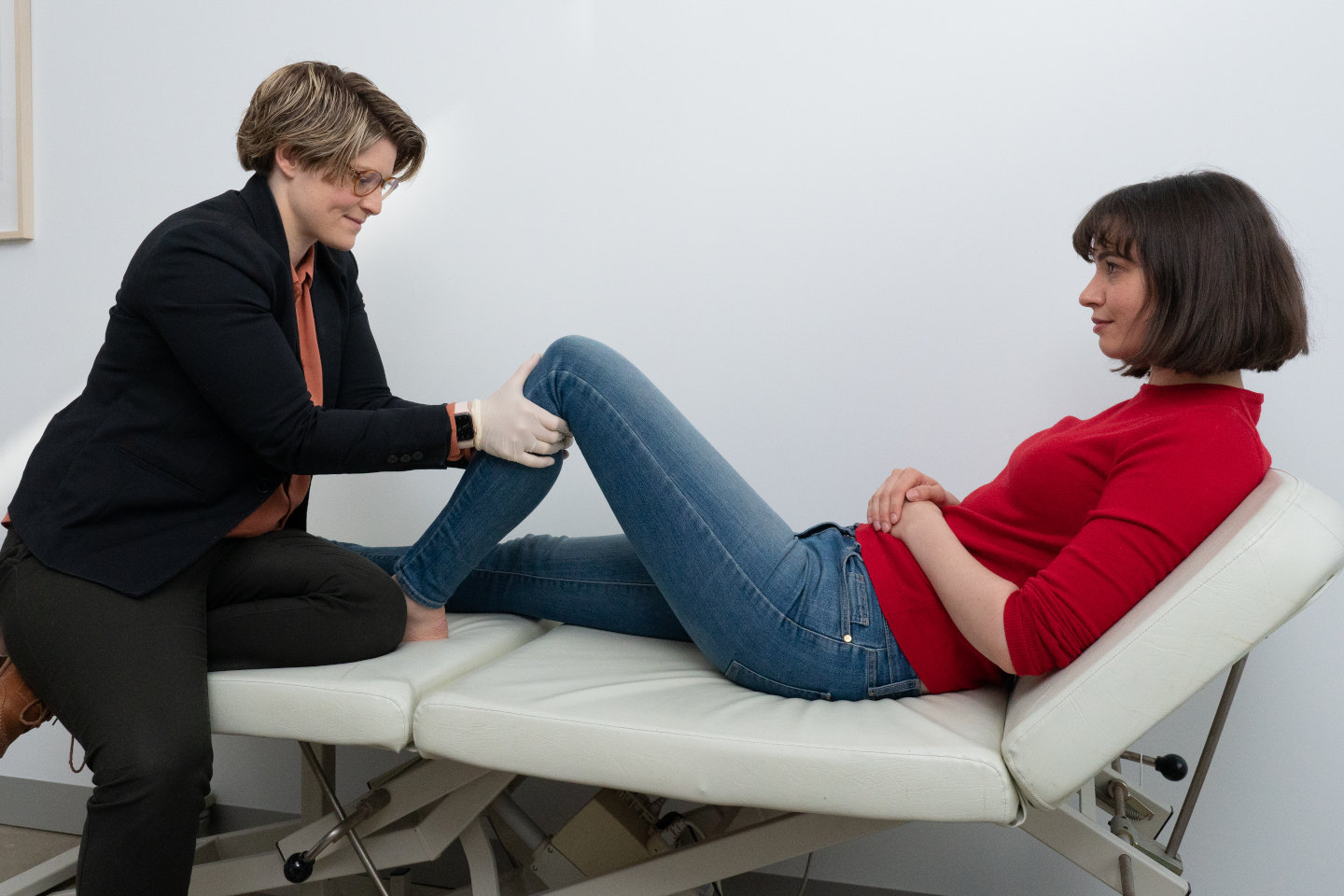
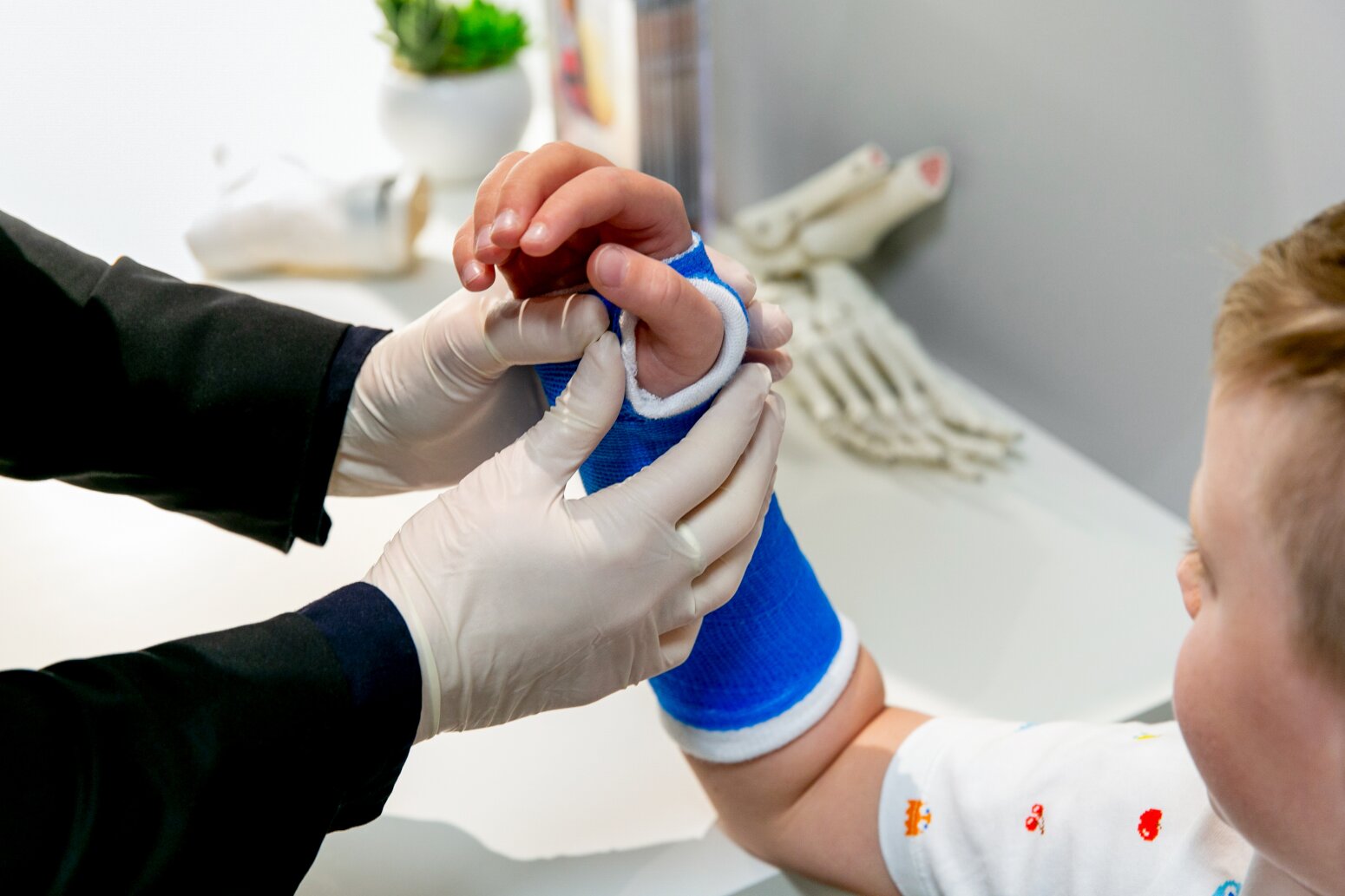

Types of Braces for Contracture Management:
There are 3 main categories of prescriptions for contracture management:
1. Static Splinting:
Static splints are designed to hold a joint in a specific position that has been gained through therapy. These braces help maintain the joint’s current range of motion and are suitable for individuals who require stability and support.
2. Serial Casting:
Serial casting involves using casts to gradually increase the range of motion in a joint. The process includes casting a limb in a better position, leaving it for some time, and then repeating the cast to achieve further range of motion. This repetitive procedure helps improve joint flexibility..
Serial casts can be “bivalved,” meaning they are cut and then reattached with straps, making them removable and lowering the risk in certain situations, such as during extended periods without immediate medical access.
3. Dynamic Splinting:
Dynamic splints are considered the most effective option in modern contracture management. These braces utilise a flexible, dynamic joint that provides a constant, low load force to stretch the joint gradually.
The person wearing the brace can still perform daily activities while the joint receives continuous passive stretching. These braces are custom-made and highly adjustable to suit individual needs and comfort levels.
Adjustable Force and Regular Monitoring:
Dynamic splints come with an adjustable force system. The force level can be modified over time to gradually increase stretching as the joint gains more flexibility.
Regular monitoring and adjustments are essential due to the risk of pressure on the skin and tissues resulting from opposing forces applied by the brace and the person’s movement.
Balancing Range of Motion and Force:
The range of motion refers to the degrees through which the joint can move.
The goal is to achieve a full range of motion to bring the joint back to a normal level of flexibility. Orthotists carefully balance the force applied by the brace with the person’s ability to tolerate it. Additionally, the design of the brace, including padding and shell, is crucial to avoid pressure injuries.


Custom Prescriptions for Contracture Management
After the assessment, Orthotics Plus has the ability to create custom equipment for our patients, these are namely:
Custom-Made Dynamic Splints for Effective Contracture Management:
Dynamic splints are commonly custom-made to suit the severity and location of the contracture. Depending on the affected body part, Orthotists may need to take a cast of the arm or ankle to create a personalised splint. During fabrication, careful consideration is given to the placement of shells and straps to apply the desired force for stretching the joint effectively.
Tailored Padding:
To ensure patient comfort and prevent pressure-related issues, our Orthotists meticulously pad the splint. Adequate padding is essential to minimize the risk of pressure areas developing on the skin or underlying tissues due to the brace’s constant low load force.
Padding can be made from EVA, cotton, lambswool or other materials which wick moisture away and distribute force effectively. Maintaining hygiene by having these materials cleanable or removable is important.
Fitting and Regular Reviews:
Once the dynamic splint is fabricated, patients return for a fitting. During this session, we finalise the fit, comfort, and functionality of the splint. Subsequent regular reviews are conducted to monitor progress in terms of improving ROM and to ensure that the pressure areas remain tolerable.


Contracture Support Services – Get Started with Orthotics Plus
Orthotics Plus works with paediatric and adult patients throughout Melbourne.
- We have multiple clinic locations
- Our qualified staff are experienced with a range of physical and neurological conditions
- We are NDIS registered
- We create custom solutions to you or your loved ones needs
To get started, please contact one of our clinics today.

Contracture Management FAQ
The question of whether contractures are preventable is a complex topic, particularly in neurological (namely stroke) settings.
Post stroke a typical foot posture often involves plantar flexion and inversion. Some physiotherapists may prefer not to use braces and instead focus on helping patients achieve a better foot position without external support.
On the other hand, there may be a leaning towards using braces to maintain the foot in the best possible position while the patient works towards achieving improved posture and focusing on rehabilitating other more proximal muscle groups. This approach aims to prevent contractures and facilitate learning to walk with a more favourable foot posture.
The matter remains controversial due to differing opinions on the most effective approach. One perspective suggests that early orthotic intervention could be beneficial in avoiding contracture development.
On the contrary, others may advocate for providing more time for physiotherapy to rehabilitate foot posture and allow more neuroplastic healing before considering orthotic intervention.
During this time we have to balance patient wants, short-term vs long-term goals, gait safety, comfort and level of support.
This is an example of the importance of patient-centred care and actively listening to treatment feedback.
It is essential to acknowledge that individual responses and needs vary, and there might be cases where the ideal preventive strategy differs from patient to patient.
Prompt evaluation and management decisions by healthcare professionals are crucial to optimise outcomes.