Orthotic Management of Ankle Conditions
Orthotics Plus treats a range of ankle conditions. We are contacted by individuals who are self-referring as well as local GPs and surgeons.
We are predominantly involved with post-operative, acute injury management and chronic issues of the ankle and supporting our clients to rehabilitation.
We provide ankle bracing (such as moon boots) and casting, and then for more complex ankle conditions, we may treat these with a range of Orthoses, namely AFOs and custom foot orthotics.
Our services take place at two clinics in Melbourne. Please contact us for a holistic, individualised treatment for your ankle.
Ankle Supports Available
-
Learn More +
Moon / CAM Boots
Custom Moon Boots

-
Learn More +
AFOs
Ankle Foot Orthoses (AFO)

-
Learn More +
Charcot Restraint Orthotic Walker
Diabetic Support

-
Learn More +
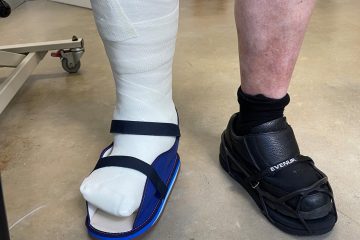
Total Contact Cast
For Ulcers / Charcot Foot
-
Learn More +
Fibreglass Casts
Treat Fractures of Upper/Lower Limbs

-
Learn More +
Night Splints
Least Bulky Night Splint

-
Learn More +
ASO Brace
Ankle Stabilising Orthosis

-
Learn More +
Arizona Lace Up Ankle Brace
Between an AFO and Ankle Brace

-
Learn More +
Carbon Fibre AFO
Lightweight AFO

-
Learn More +
Shin Splints
Support at Orthotics Plus

-
Learn More +
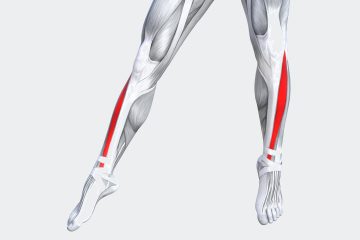
Tibialis Anterior Dysfunction Tendonitis
Treatment for Tibialis Anterior Pain
-
Learn More +
Peroneal Tendonitis
Treatment for Peroneal Tendonitis

-
Learn More +
Ankle Sprain
Sprain Healthcare & Equipment
-
Learn More +
Achilles Tendonitis
Achilles Tendonitis Treatment

-
Learn More +
Achilles Tendon Rupture
Conservative Management of Ruptures

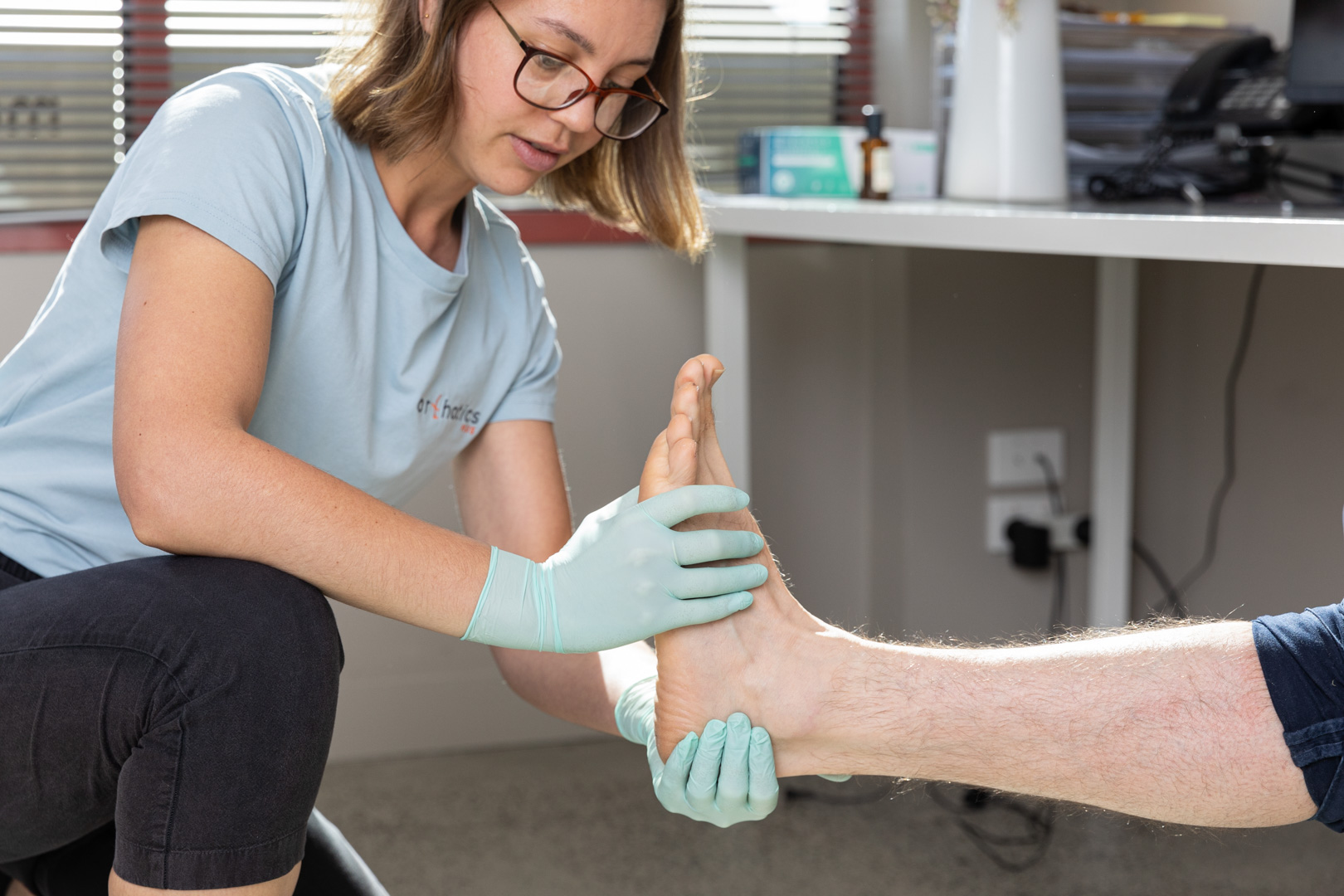
Ankle Assessments
The first step to ankle rehabilitation is to complete a comprehensive assessment. Our Orthotists will talk through the patient’s medical history and consider:
- Addressing immediate symptoms (often pain management)
- Testing ankle range of motion, strength, balance, posture while standing and walking
- Strategies or interventions already used to manage the ankle condition
The relevant anatomy for ankle assessments is namely the talocrural joint (tibia, fibula & talus) which controls dorsiflexion and plantar flexion, as well as the subtalar joint, which controls inversion and eversion.
We will formulate a treatment for the patient’s respective condition. The ideal outcome of working with Orthotics Plus is to improve comfort, safety and functional outcomes.

Customised Ankle Equipment, Trials & Funding
After your assessment, you may be provided with recommendations for certain ankle braces, Orthotics or other equipment.
Orthotics Plus advocates for patient choice and control, we will endeavour to safeguard your decisions and financial preferences without compromising the quality of treatment.
Patients can express their preferences on the material (i.e. wish to invest in carbon fibre), colours, styles and we will accommodate that as best as possible.
Certain types of equipment can be trialled on the day, however, this is not always possible. For high-cost equipment (i.e. FES), a longer trial period may be considered.
Ankle FAQ
Yes.
A prerequisite of this is to firstly recommend Orthotics in different tiers of management, such as recommending the cheapest, lowest risks options first.
We provide ongoing options and education surrounding equipment, so the patient can choose with an informed decision.
For example, a patient may visit and choose a regular AFO model. After some time, the patient loves the AFO and wishes to upgrade this to a carbon-fibre model.
In this case, we would use the cast we already have on file, or retake a new cast, then make a new model AFO exactly the same.
Follow-up appointments will be recommended by your Orthotist.
In these appointments, we will reassess if what we’re trying to achieve has been achieved, namely the management of symptoms and improving daily life/function.
The equipment’s condition and settings will be reviewed.
We would suggest the most common ankle referrals relate to:
- Ankle osteoarthritis
- Foot drop
- Lateral ligament injuries
- ASOs
- Moon boots
- Tibialis posterior dysfunction (severe pronated feet)
- General ankle pain
This varies depending on the condition.
If it’s an osteoarthritic ankle, our suggestions will be based on the severity of the condition.
Early osteoarthritis may respond well to support, adjustments in ankle posture with orthotics and an exercise program as well as other interventions such as medications. Late stage osteoarthritis, where other interventions have been unsuccessful, may respond well to reducing movement and controlling the ankle joint. This is often in lieu or a precursor to an ankle fusion.
For ligament injuries, typically we will work collaboratively with a Physiotherapist but provide an environment of functional healing. This is where the damaged ligament is protected during the early phases of healing. Many ligaments respond well to appropriate loading during the healing process, but too much and excessive movement can be detrimental.
For fractures, typically there is no exercise prescription during the acute phase, however after the cast is removed, we would recommend a Physio or rehabilitation specialist. We may also prescribe a basic range of motion exercises.
For those who have been immobilised for a long time, a less conservative brace may be suggested to allow confidence to build back in the injured limb.
E.g. for a patient coming out of a lower limb cast after 8 weeks, wearing an ASO might make the patient feel more stable and provide the confidence to progress more quickly with their rehabilitation program. It may also protect the injured and weaker ankle from re-injury during the early phases and during their return to sport if this is their goal.
Our Orthotists will provide you this information during your assessment.
The answer to this depends on why the patient is falling.
For people falling as a result of decreased strength in the lower limb, we are likely to make an enormous difference within one session.
In contrast, if that person is falling due to poor eyesight or complications with prescription medication, then that would be outside the scope of our Orthotists.
Orthotics Plus will always provide our recommendations from a holistic perspective, such as recommending undertaking a falls prevention program.