Support at Orthotics Plus
Foot Drop is an umbrella term for the symptoms a person experiences who is unable to lift their foot upwards (a movement called dorsiflexion).
Foot drop is not a condition or disease in itself. Foot drop is typically a symptom of an underlying neurological, muscular, or anatomical problem.
Orthotics Plus provides support for paediatric (under 18) and adults (over18) who are living with foot drop. We are experienced with a range of physical and neurological conditions.
Our healthcare services are available at two locations in Melbourne: Malvern & Heidelberg.

What is Foot Drop?
Foot drop is typically a sign of an underlying neurological, muscular, or anatomical problem.
It is the inability to lift the front part of the foot up towards the shin, which means people may catch their foot on the ground/obstacles as they walk. It can affect all ages.
The primary anatomy to consider is tibialis anterior, the peroneals and the long toe extensors.

Symptoms of Foot Drop
People may inadvertently contact the ground with their toes or forefoot when swinging the leg through and also contact the floor with their forefoot instead of their heel when the foot lands, this is an inefficient way of walking and potentially dangerous.
Foot drop may also cause gait deviations/adaptations which create lower back, knee or hip pain People who are living with foot drop are at higher risk of falls.
Foot drop may or may not be associated with other issues such as weakness of the calf muscles (plantar flexors), muscles around the knee (knee extensors) and other muscle groups.
These are considered by our expert clinicians when deciding on an ideal prescription for foot drop.

Causes
Foot drop can be due to a number of factors. These can be separated into ‘structural issues’, ‘upper motor neuron lesions’ and ‘lower motor neuron lesions’.
Structural
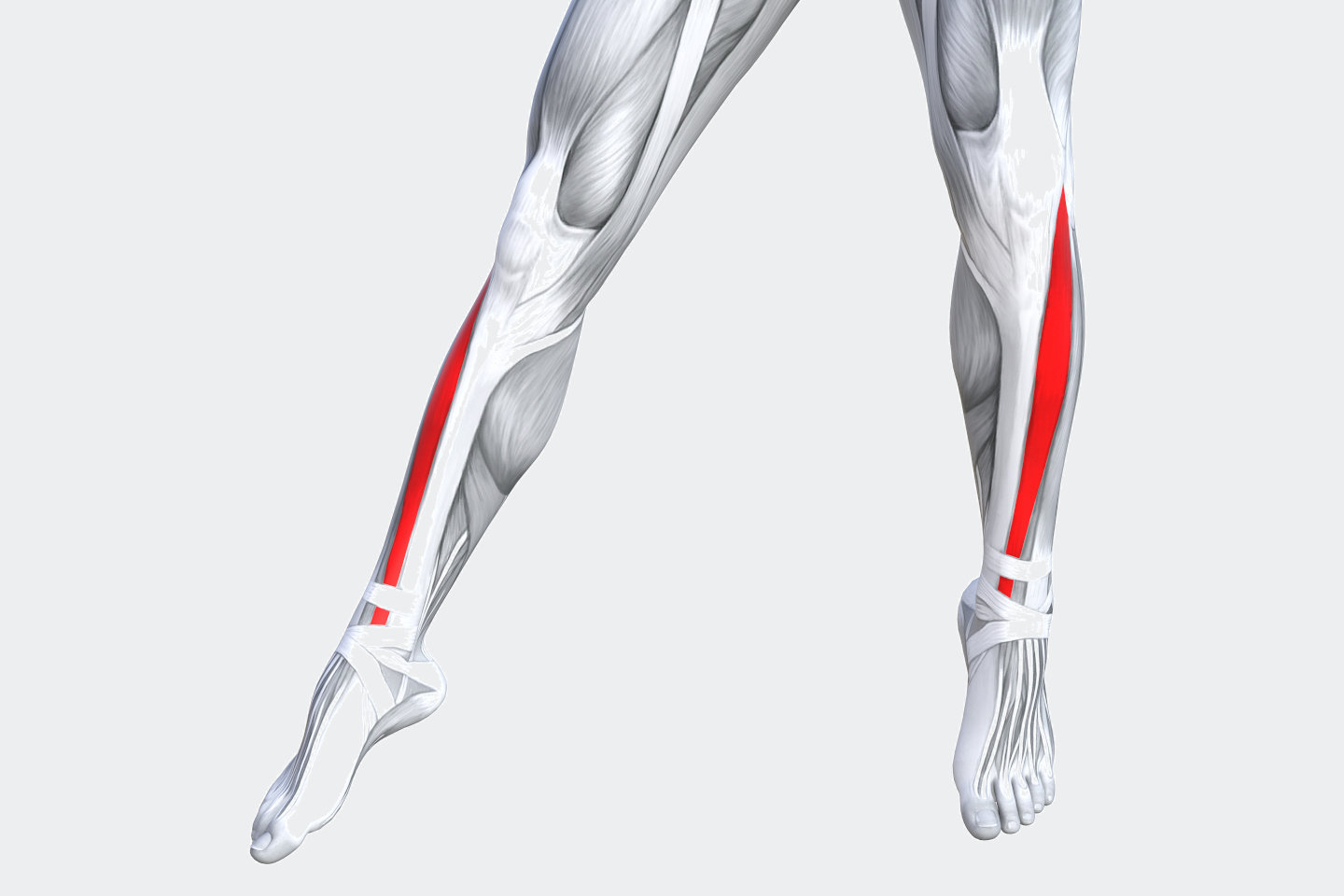
A structural issue is a problem with the anatomy, for example, the tibialis anterior tendon has been severed or the muscle has been damaged.
This presentation is less common.
Upper Motor Neuron Lesion
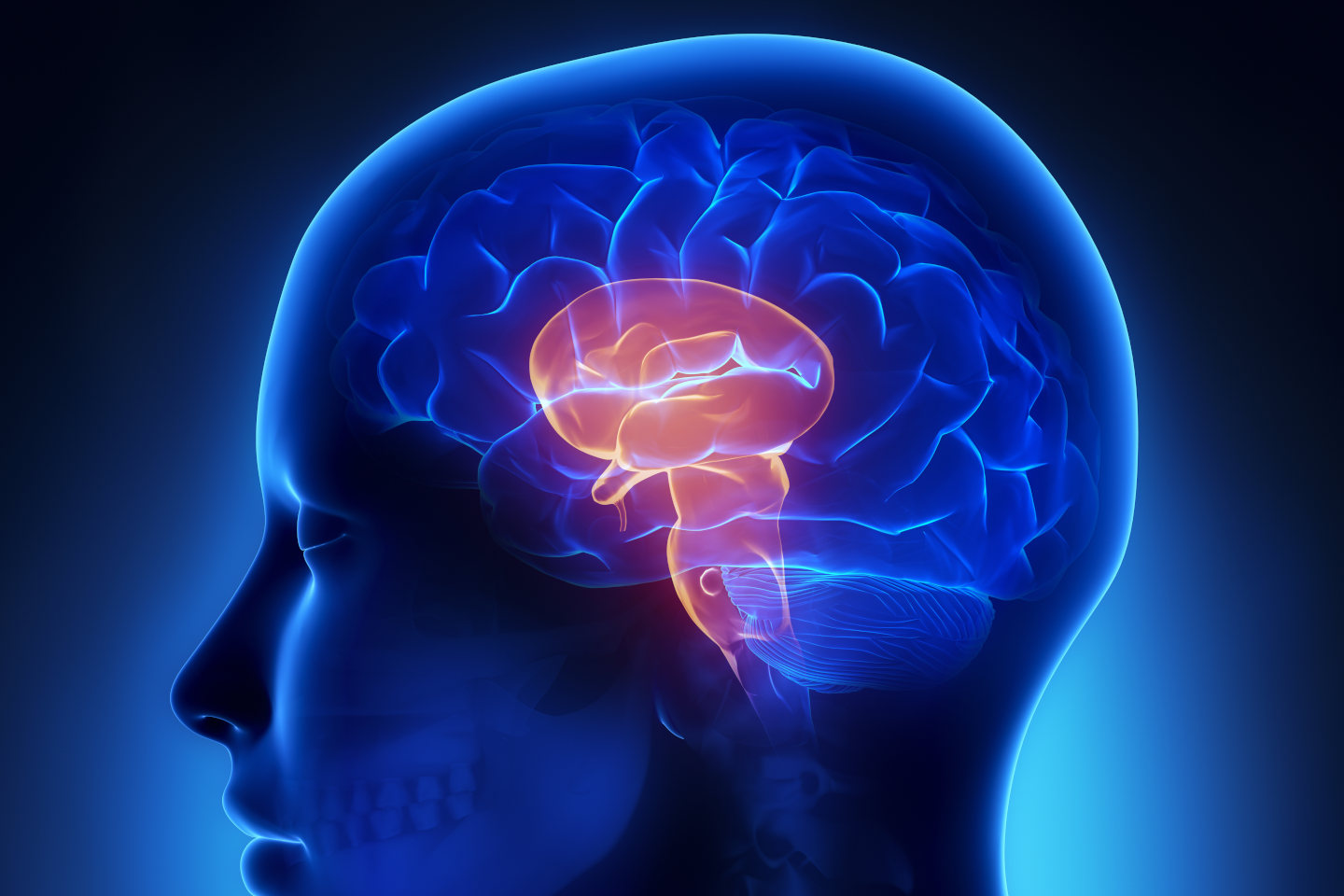
Upper motor neurons are found in the brain and spinal cord and transmit regulatory information as well as movement information to the lower motor neurons.
Damage or an ‘upper motor neuron lesion’ (UMNL) in this part of the central nervous system may result in a more complex presentation such as spasticity as well as foot drop.
Examples include stroke, MS, cerebral palsy.
Lower Motor Neuron Lesion
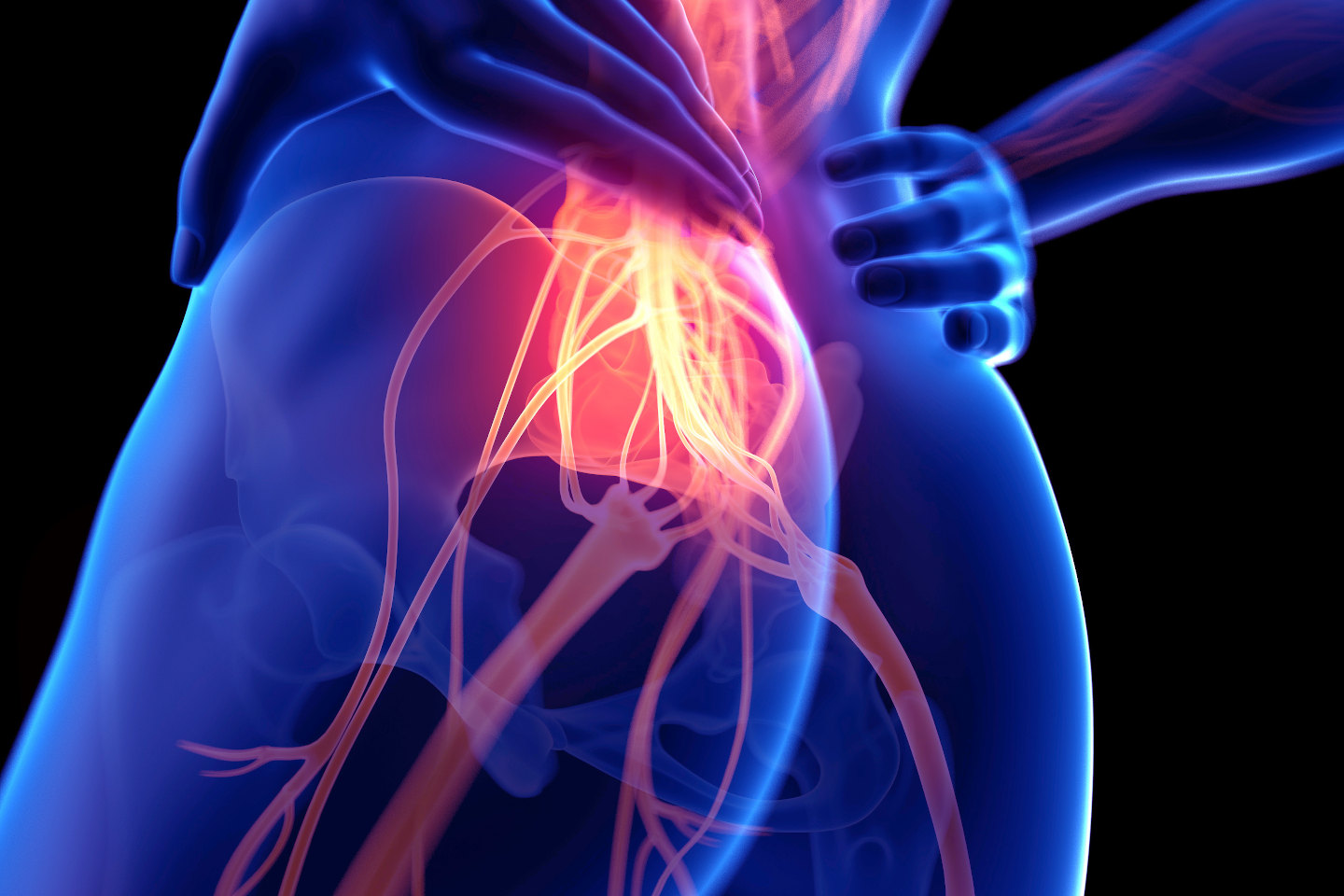
Lower motor neuron lesions (LMNL) occur lower in the spinal cord and between the spinal cord and muscle.
For example, if the nerve controlling the tibialis anterior muscle is damaged near the muscle, the signal can’t reach the muscle fibers and will cause foot drop. This presentation is usually a flaccid paralysis or weakness rather than spasticity.
Examples include polio, ALS, traumatic peripheral nerve damage.
To simplify, foot drop occurs when the affected muscles cannot output optimal amounts of force to lift the limb.
Severities
The way a person experiences the symptoms is varied.
For example, there is flaccid foot drop, where the person cannot move their foot at all.
There are also cases where a person has weakness and fatigues rapidly, where they may be fine in the morning yet at high risk in the evening.
It is also common that people with upper motor neuron issues (such as with stroke, cerebral palsy etc) will experience spasticity and altered reflexes which we need to consider when looking at a prescription.
There are also fractures, strength levels and other concurrent disabilities to consider.

Foot Drop Assessment & Treatment
We work with both paediatric and adult patients. During the appointment, we will perform a subjective and objective assessment.
There’s a large range of different orthotic options to consider.These can often be trialled in the clinic during an appointment.
Together, we can come up with an appropriate prescription based on the person’s lifestyle, the shoes they wear, their activity levels and what is clinically best for them.
It is Orthotics Plus’ goal to enable the foot drop community to walk better with greater safety.
Orthotics for Foot Drop
Relevant Orthoses that may be considered in the conservative management of foot drop are:
- Functional Electrical Stimulation (FES)
- Leaf spring AFO
- Jointed AFO
- GRAFO
- Solid AFO
- Carbon fibre AFO
- Foot Up
- PDE
We believe the role of an Orthotist is one aspect of support in the holistic management of foot drop as we can provide an immediate difference in a patient’s safety and walking ability.

Multidisiplinary Care
We typically work alongside Physiotherapists to maximise how effective our equipment can be, an example of this is addressing other weaknesses that can be maintained or improved.
For patients in the early phases of rehabilitation, we provide the minimal intervention possible and will encourage the use of devices to enhance neuroplasticity and recovery.

University Qualified, Experienced Clinicians
Since 2012, it has been our mission to help the Melbourne community to live their very best lives.
We believe improvements in mobility make a difference for quality of life and being ready to move forwards.
We tailor our approach to your circumstances and believe in a patient-centered model of care.
We perform our assessment and provide recommendations on what we believe is clinically appropriate. We are active listeners – if the patient isn’t satisfied with a specific option, we will take that into account and work together to find an option they’re happy with.
We also help our patients with equipment trials to help safeguard their decisions.

Selecting A Device for Foot Drop
It is common for patients to have been prescribed a device many years ago and to have not updated this.
We would encourage patients to contact Orthotics Plus to investigate what other options may be available for themselves or their loved ones.
Technology has improved rapidly and NDIS funding options allow us to prescribe the device we feel will allow the patient to achieve their goals and function the most effectively.
Additionally, our experienced clinicians may provide additional information or have different ideas which can help you or your loved one.

Referrals for Orthotics Plus
Orthotics Plus has a wealth of experience treating foot drop as a result of different causes, whether it be neuromuscular, traumatic, or other.
- We are registered Orthotists with AOPA
- We operate under a variety of funding schemes, including the NDIS
- We are kind and compassionate
- Our administration team is prompt and friendly
- We advocate for choice and control
To get started with Orthotics Plus, please use our clinic locations or referrals pages.

Read Related Success Stories
We worked with a lovely lady who is very inspirational!
The client had foot drop as a result of a stroke she experienced in the years earlier. She could not walk without a gait aid and didn’t feel safe walking without rails.
We recommended a Functional Electrical Stimulation orthosis and intense physiotherapy.
Not too long after, she achieved the amazing goal of walking 8 kilometers independently. This is a brilliant outcome!
Orthotics Plus is grateful for our opportunity to work with hundreds of cases involving foot drop.
One such example is a patient presenting with isolated foot drop caused by spinal surgery. The patient was hip hiking to prevent from catching their toes which was causing fatigue as well as back pain.
In this case we suggested a carbon fibre leaf spring AFO, which is lightweight and low profile. Fitted on top was a custom foot orthosis for comfort.
The immediate change in walking pattern was obvious and the patient could swing their leg through without hitting their toes on the floor as the AFO supported her.
As the patient had developed some bad habits due to walking this way for years, her gait deviations took several months time to normalise.
But with consistent walking and physiotherapy her deviations were reduced to a barely noticeable level and her back pain improved.