Orthotic Treatment of Plantar Fasciitis
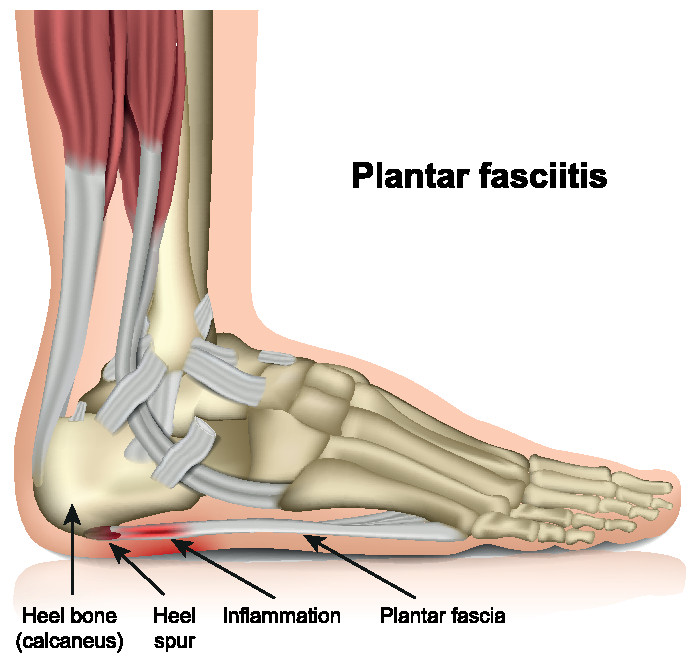
Plantar Fasciitis is inflammation of the attachment point of the plantar fascia (fibrous tissue/aponeurosis) to the calcaneus (a bone in the heel) and can occur for a number of reasons, with the most common being excessive loading.
At Orthotics Plus, we primarily treat plantar fasciitis with either custom foot orthotics or silicone heel cushions combined with a significant calf and plantar fascia stretching program. We take a holistic approach to treating plantar fasciitis and often refer patients for other intervention if we feel it is required.
As orthotists, we are well-placed to assist patients with plantar fasciitis, with the ideal outcome being that the patient makes a full recovery.
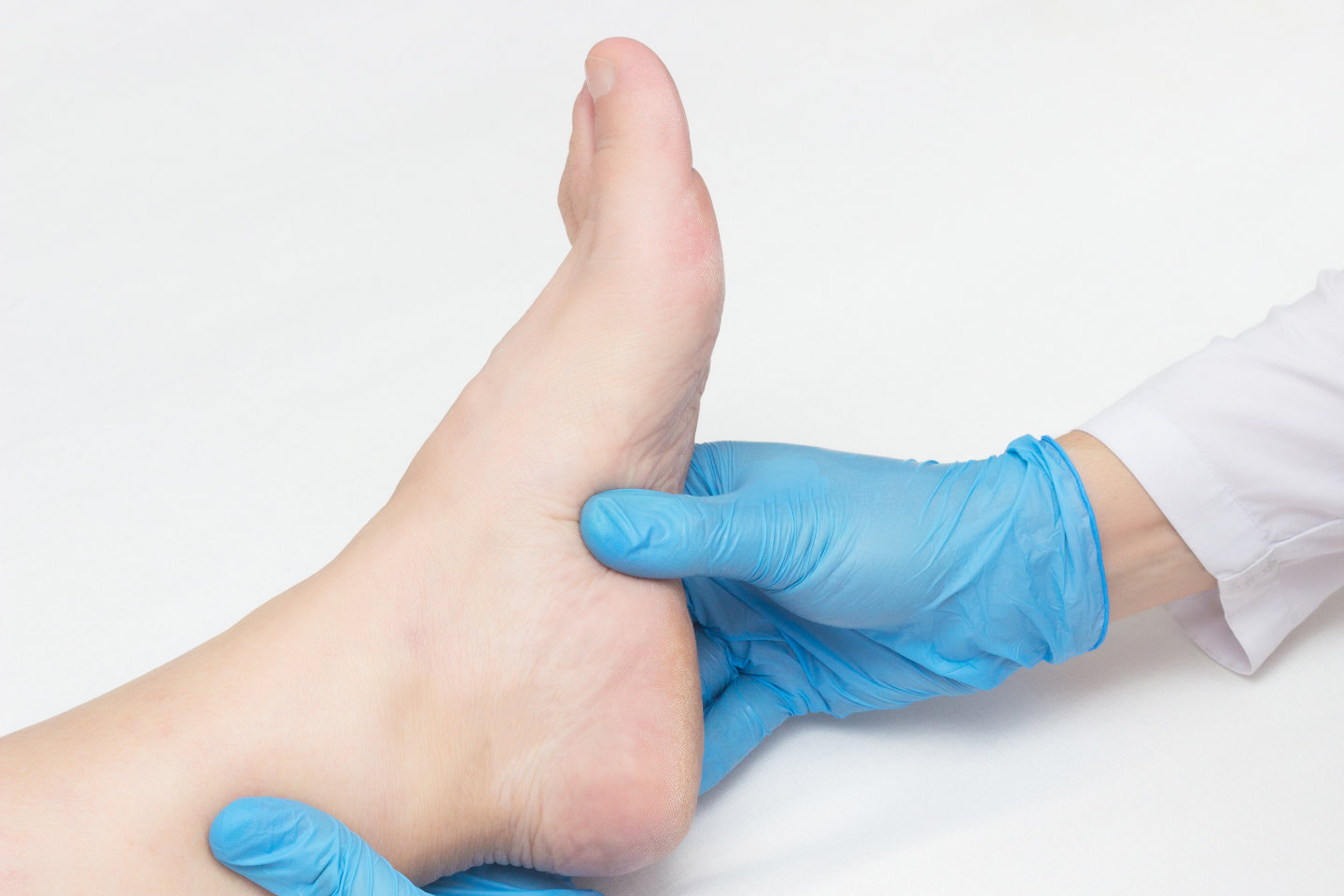
Orthotics for Plantar Fasciitis
As mentioned, the condition is usually treated through either foot orthotics or silicone heel cushions, sometimes night splints. These treatment pathways should be combined with ideal changes to lifestyle, footwear, education and support.
Custom Foot Orthotics
Foot orthotics are used when there is a biomechanical issue contributing to the plantar fasciitis.
For example, for patients with a medial arch collapse or a pronated foot, we would design a custom orthotic with medial arch support and cushioning of the heel area.
This would simultaneously treat the biomechanical issue as well as provide cushioning to the heel area.
Silicone Heel Cushion
These are most appropriate for patients experiencing milder symptoms and show no signs of biomechanical abnormality.
Silicone heel cushions are located in the heel, so they are worn by people who do not require arch support in the midfoot.
The cushion raises the heel to reduce the tension on the Achilles tendon and the plantar fascia.
Night Splints
Night splints (also known as a Strassburg sock) are used rarely and only in very severe cases of plantar fasciitis.
This is an Orthotic device that is worn on the foot and connects to the lower leg.
It is typically worn whilst sleeping and delivers a constant stretch to the calf, achilles and plantar fascia.
Lifestyle Factors that Contribute to Plantar Fasciitis
There are many causative and correlative factors that can cause and worsen plantar fasciitis, such as:
- Weight gain, notably in pregnant women
- Changes to the surface walked on most commonly (ie: soft carpet to concrete floors)
- Overly sedentary/active employment
- Changes in footwear
- Rapidly increased loading (i.e too much running)
- Worsened strength levels or mobility
When working with Orthotics Plus, we’ll review the lifestyle factors which we have control over, then modify them as necessary.
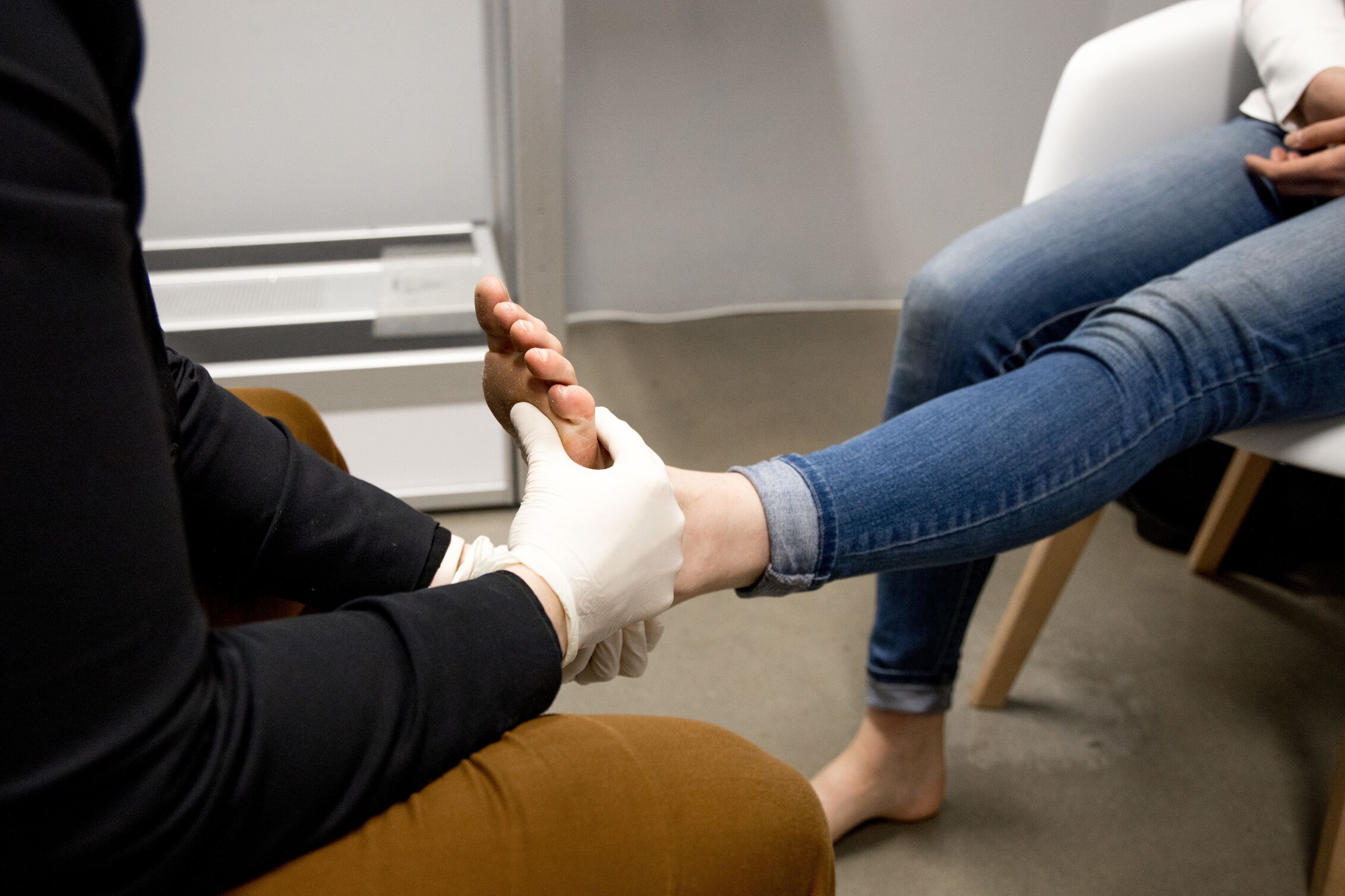
Plantar Fasciitis Treatment at Orthotics Plus
At Orthotics Plus, we offer both Podiatry and Orthotic services for this condition. Both are appropriate pathways. Typically, an Orthotist is preferred if there is an underlying biomechanical issue.
The patient will visit Orthotics Plus and we perform an assessment to identify the cause of the condition. This includes range of motion and strength testing to discover additional deficiencies to be addressed.
A diagnosis will be formalised and we will discuss the appropriate treatment pathway with the patient, which is generally a combination of Orthotics, lifestyle modifications, education, multidisciplinary care and follow up support.
We have cases where patients have made a full recovery in 4-6 weeks, however, this can vary depending on how long the condition has been present.
Referrals for Orthotics Plus
Please make a booking through our clinic locations or referrals pages to start the process.
- We have two clinic locations in Melbourne
- We have over 10 years experience treating plantar fasciitis
- We listen and adopt patient-directed care
- We are fully Australian owned and operated
We encourage people to seek help as soon as possible, the longer you’ve had plantar fasciitis, the harder it is to rehabilitate. We look forward to working with you!

Plantar Fasciitis FAQ
We firstly suggest not to ignore the condition, and seek medical advice from your GP and Orthotist for treatment as soon as possible.
In most cases, excessive rest, excessive weight bearing and repeating suboptimal routines are things that we would suggest to avoid.
At Orthotics Plus, we do not push people towards a specific brand of shoe.
We typically recommend a shoe that has a sound cushioning with a little bit of height under the heel. The patient’s feet should feel stable and secure.
Additionally, we recommend a shoe that complements a person’s foot posture. For example, if someone has a supinated foot posture, then perhaps a higher arching shoe will work best.
We typically do not recommend totally flat shoes.
We have seen patients benefit from the use of ice or heat packs.
Often we suggest patients to freeze a water bottle and give themselves an ice massage, as the bottle allows people to roll their foot in a back and forth motion.
At Orthotics Plus we will prescribe a regime we have tailored over the years which will aim to stretch and strengthen the surrounding tissues and aim to solve the root cause of the issue.
If we believe you need a more in-depth regime we will refer you to the appropriate professional.
We see many patients benefit from the strengthening and stretching of both the foot and calf, particularly the posterior complex (referred to as the gastroc-soleus complex) which can reduce the load off the plantar fascia.
No, they are not the same. This is a misconception.
It is possible for someone to have one or the other, or both of these simultaneously.
It is important to note that an X-ray mayshow a heel spur, however this imaging would be useless in regards to the diagnosis of plantar fasciitis.

